Grounded in science. Driven by purpose.
Educating to advance the power of nutrition for human and planetary health.
Loews Coronado | San Diego, CA | May 14-17, 2026
Where Science Meets Solutions for Human and Planetary Health
Power Of The Plate is the evolution of PBNHC —expanding a decade of scientific rigor into a cross-sector movement. Still anchored in world-class, CME/CE-accredited education for clinicians, the conference now draws leaders from public health, food systems, sustainability, education, policy, and industry.
What makes this gathering unique is its recognition of the full interconnectedness of the Power of the Plate—how we grow, produce, and consume food shapes not only individual health, but the health of communities, economies, and ecosystems.






Free Download!
Plant-Based Nutrition Quick Start Guides
New to plant-based nutrition? Download our comprehensive Quick Start Guides and get the tools you need to begin your journey with confidence.

Planting the Seeds Of Change
When healthcare professionals and changemakers embrace and advance the regenerative Power of the Plate, they ignite broad dietary and cultural shifts—preventing disease, transforming food systems, restoring planetary health, and uniting communities for a healthier future.

Virtual & in-Person Events
Events that connect healthcare professionals and leaders to advance the Power of the Plate.

Plantrician Library
Evidence-based articles and patient fact sheets from our Plantrician Providers Library.

Regenerative Agriculture
Healthy soil, healthy food, healthy people, healthy planet.
Fuel the Movement. Transform the Future.
Join the movement! Together we can leverage the Power of the Plate to transform health, healthcare, and our food systems—for people and the planet. Your support fuels this vision, and fundraising is the vital force that makes our work possible.
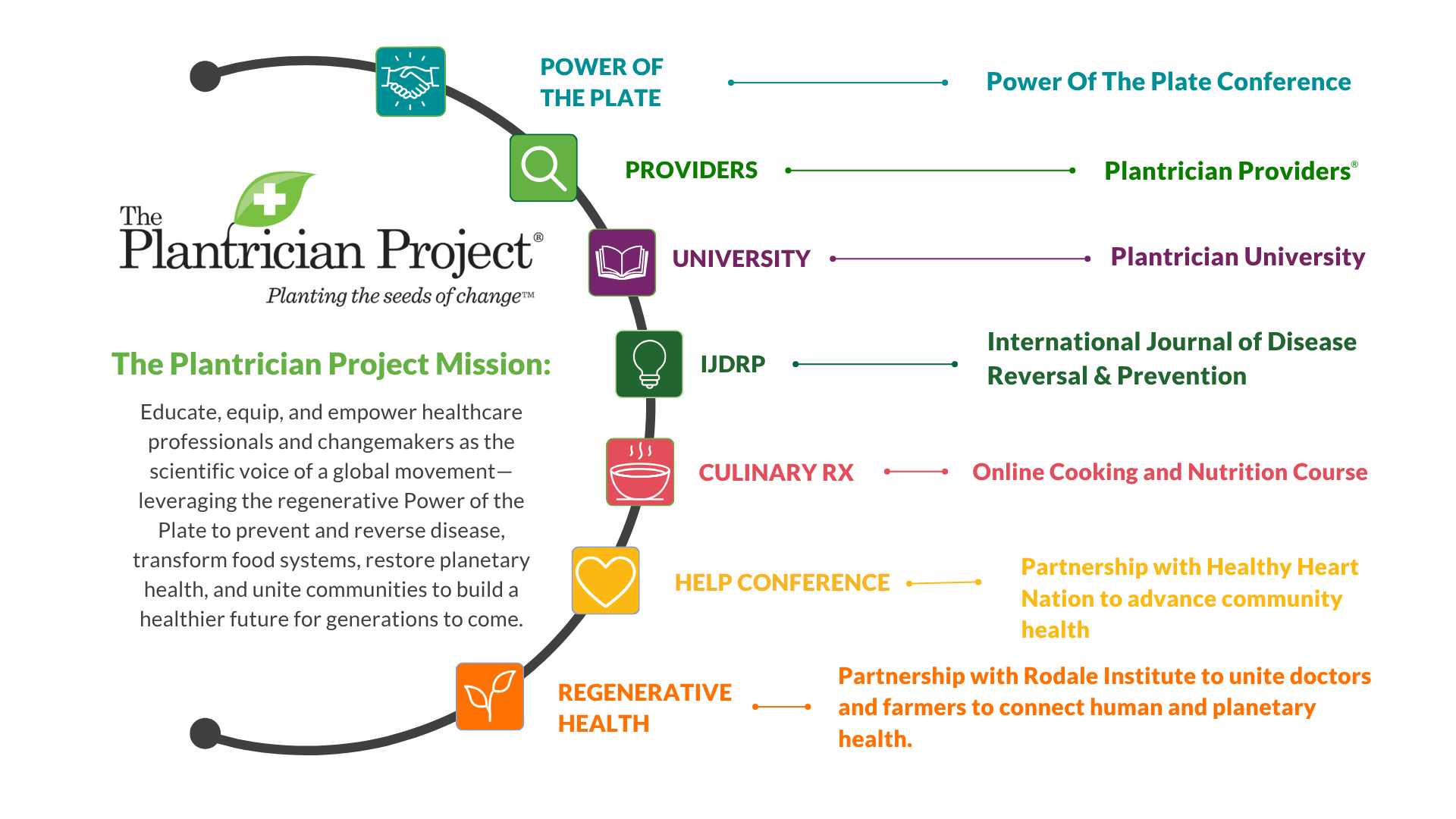
Plantrician Resources & Initiatives

Power Of The Plate Conference
The global gathering where science becomes action across health, food systems, and sustainability—rooted in regenerative solutions and CME/CE-accredited education.

The IJDRP
A free, open access, peer reviewed journal created to document the science of nutrition and lifestyle to prevent, suspend and reverse disease

Plantrician Providers
Plantrician Providers is a global directory of healthcare professionals who champion the Power of the Plate—applying nutritional science to prevent, halt, and often reverse chronic disease.

Plantrician University
Education platform empowering healthcare professionals and changemakers with the knowledge and tools to use nutrition to prevent disease and advance human and planetary health.

Quick Start Guides
Learn how and why adopting a whole food, plant-based dietary lifestyle can help you, your family, and your patients achieve optimal health and well-being

Healing Healthcare Manual
Healing Healthcare: A Guide for Transforming Healthcare Systems Through Plant-Based Nutrition and Lifestyle Medicine
Experts Agree
Subscribe To Our Newsletter
Copyright © 2026 The Plantrician Project. All Rights Reserved.





